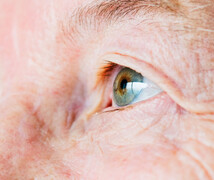
Keratoconus is a progressive eye disease that can cause blurry vision, irregular astigmatism, light sensitivity, and other symptoms. Here, Duke cornea specialist Melissa Daluvoy, MD, explains what you need to know about this corneal disease and the types of treatments available.
What Is Keratoconus?
Keratoconus is a weakening and thinning of the cornea (the front surface of the eye). It can occur in one or both eyes. As the disease advances, the cornea begins to bulge outward, taking on the shape of a football -- as opposed to the round basketball shape of a healthy eye. Keratoconus often begins in adolescence or early adulthood and progresses until a person is in their 40s or 50s, although the rate of change varies from person to person.
What Causes Keratoconus?
No one is sure exactly what causes keratoconus. It appears to run in families but also may have some environmental influences. There is some evidence to suggest it may be related to chronic eye rubbing, which can make keratoconus progress faster. Certain populations have a higher incidence of keratoconus. For instance, 5 to 15% of people with Down syndrome have the disease.
What Are the Signs of Keratoconus?
Keratoconus can cause blurred vision, frequent changes to your glasses or contact lens prescription, halos at night, streaking of lights, and sensitivity to light. Regular eye exams can identify keratoconus early, but you should see your eye doctor promptly if you experience vision changes, glare, distortion, halos, or light streaking or see ghost-like images. People with Down syndrome or who have other special needs may not report early changes in vision, so it is important to schedule regular eye exams and to screen for keratoconus during their teen and early adult years.
Early detection allows the greatest number of treatment options, including the chance to halt the progression of keratoconus.
How Is Keratoconus Treated?
Most people with keratoconus need help to see clearly. Glasses and traditional contact lenses can be effective for mild vision problems. For more advanced cases, specialty contact lenses may be recommended. When sufficient vision correction cannot be achieved with glasses or contacts, doctors can insert corneal rings -- called Intacs -- to improve vision. If keratoconus continues to progress, a corneal transplant may be necessary.
Can Anything Stop the Progression of Keratoconus?
While there are no treatments to prevent or reverse the disease, collagen cross-linking can halt its progression, preserve vision, and delay or prevent the need for a corneal transplant. Duke was the first hospital in North Carolina to perform this FDA-approved procedure, which strengthens collagen in the eye. Because the cornea stiffens with age, ideal candidates for collagen cross-linking are typically in their 40s or younger.