Conflicting mammogram guidelines may leave many people unsure about when and how often to be screened for breast cancer. Jay Baker, MD, a Duke Health breast imaging specialist, answers six questions about mammograms you should be asking so you know when to schedule your first--or next--mammogram.
Is Getting a Mammogram Worth the Risks?
Some people may question whether the benefits of mammography outweigh possible risks. For instance, mammograms can identify abnormalities that turn out not to be cancer. This can result in additional testing, visits, and sometimes procedures, which can cause stress and anxiety. Mammography also exposes people to a small amount of radiation, although the amount is so small that the actual risk, if any, is too small to measure.
However, regular mammograms are the best way to detect breast cancer at the earliest-possible stage. They identify cancer before symptoms (such as feeling a lump) occur. Early cancers found on a mammogram are often small, confined to the breast (meaning they haven’t spread to other areas), and can be the easiest to treat.
Bottom line: Having routine screening mammograms reduces the risk of dying from breast cancer by 40% or more, so getting screened is well worth the small potential risk, said Dr. Baker.
At What Age Should I Start Regular Mammograms?
If you are at average risk for breast cancer, screening should start at age 40. “Everyone agrees, even those who aren’t the biggest fans of mammography, that the most lives and the most years of life are saved by starting screening at age 40. The data are very clear,” Dr. Baker said. New screening recommendations from the U.S. Preventive Services Task Force back him up. These new guidelines advise people who are assigned female at birth and are at average risk for breast cancer to begin screening at age 40, rather than 50, as previously recommended.
According to the Society for Breast Imaging, breast cancer risk starts increasing around age 40, and one in six breast cancers occurs in women between the ages of 40 and 49. Three out of four women who develop breast cancer have no family history of the disease. Other studies confirm that about half of fatal breast cancers are diagnosed before the age of 50, and about 30% of the total years of life lost to breast cancer are from women who were diagnosed in their 40s.
Bottom line: Start regular mammograms at age 40. If you are at high risk for breast cancer (that is, you carry one of the breast cancer genes, or you have a strong family history of the disease), you may benefit from starting screening before age 40, and potentially from additional screening with MRI. Speak with your primary care doctor or ob-gyn about your risk and a plan for screening. Regardless of your risk factors, if you feel a lump in your breast, schedule a mammogram immediately, no matter your age.
How Often Should I Have a Mammogram?
Screening every year saves lives and results in a 25 to 40% decrease in lives lost, explained Dr. Baker. The Society for Breast Imaging reports that the longest-running breast screening trials in history show that regular annual mammography screening -- meaning once a year -- cuts breast cancer deaths by almost a third in all women aged 40 years and older.
Annual mammograms are also important if you have been told you are at high risk for breast cancer -- because you have a family history, dense breasts, or a genetic mutation such as BRCA 1 or 2.
Bottom line: Annual mammograms increase the likelihood of catching breast cancer at the earliest stage and reduce the risk of dying prematurely of breast cancer.
At What Age Should I Stop Having Mammograms?
While some organizations suggest women over age 74 no longer need mammograms, Dr. Baker said most of the research has simply not included women 75 years and older. Rather, he said research shows there are real benefits to annual screening mammograms as long as you are in good health and have about eight to ten years of life expectancy. (For example, on average, an 80-year-old woman can expect to live until age 89, with many living even longer than that.)
Bottom line: Continue annual mammograms as long as you are healthy and anticipate having several good years of life ahead.
Should I Have a 3D Mammogram?
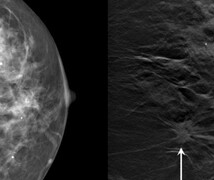
Three-dimensional mammography, also known as breast tomosynthesis, is a form of digital mammography. Unlike standard digital mammograms, which create a two-dimensional view from the top and sides of your breast tissue, 3D tomosynthesis mammograms take low-dose images from many angles using essentially the same overall radiation dose as regular 2D mammograms. A computer then reconstructs those images into a 3D image of your breast.
Research indicates 3D mammograms find 25 to 35% more breast cancers and result in up to 30% fewer false positive results. Data also show 3D mammography does a better job finding breast cancer in dense breast tissue. All Duke sites in Durham, Orange, and Wake counties offer 3D tomosynthesis for all screening and diagnostic mammograms.
Bottom line: Talk to your doctor about whether you will benefit from a 3D mammogram.
Where Can I Get a Mammogram?
Duke offers mammography in many convenient locations. Saturday appointments are also available. When choosing where to have your mammogram, consider whether the doctors reviewing your mammogram images are dedicated breast imaging radiologists. Data show breast imaging specialists find more breast cancer and have fewer false positives.