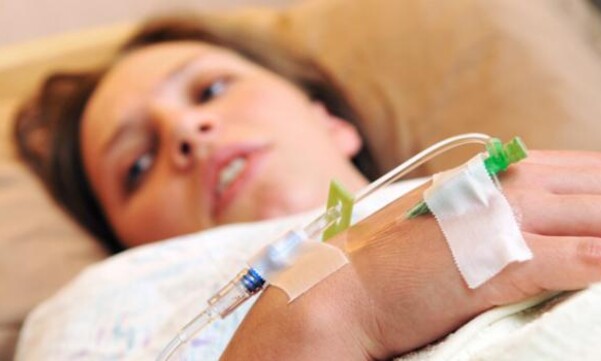
Sebastian Sancho seemed perfectly healthy when he was born in the spring of 2012. Within two months, however, he was diagnosed with chronic granulomatous disease (CGD), a rare and serious genetic disorder that left his immune system unable to fight infection. His only hope for a cure was a stem cell transplant.
The First Signs of Illness and a Frightening Diagnosis
The first indication of a medical problem surfaced when Sebastian was two months old. He spiked a high fever and was hospitalized for a few days near his home in New York City. “A dozen different specialists couldn't figure out what was going on,” said his father, Miguel Sancho. A few weeks later, he developed a skin abscess that required minor surgery. A week later, he got another, then another. Sebastian spent the next few months in and out of the hospital. Frustrated and worried, his mother, Felicia Morton, took her son to an immunologist who diagnosed Sebastian with CGD. “It was devastating,” said Sancho. “This was not a condition that could be treated and go away or one that would require moderate adjustments. It was a life-threatening genetic primary immune deficiency.”
Pursuing a Cure
In some cases, CGD can be managed with medications, vigilant medical care, and strict environmental restrictions. But even with careful oversight, many with the disease die prematurely. Only the luckiest make it to adulthood. Because Sebastian was diagnosed with the most severe form of CGD, his parents began investigating the only cure for the disease, a stem cell transplant.
Choosing Duke
Several U.S. centers perform pediatric stem cell transplants -- also known as bone marrow transplants -- but Sebastian’s parents had specific criteria. The procedure is not without serious risks, and they wanted “a place that was very good for pediatric CGD transplants. Duke had a very impressive record,” said Sancho.
They also choose Duke because as a pioneer in umbilical cord blood transplant from unrelated donors, it had decades of experience finding the best matching stem cells for patients. That was important because it can be difficult for people with a mixed ethnicity like Sebastian to find an appropriate donor. Neither Sancho, Morton, nor Sebastian’s older sister were compatible. Once they set their sights on Duke, they contacted Vinod Prasad, MD, MBBS, a Duke pediatric transplant and cellular therapy specialist.
Dr. Prasad remembers the conversation. “We get phone calls about children with complex diseases and rare disorders, patients who have been told that their transplant is too complex or that nothing much can be done. Theirs was one of those phone calls.” Dr. Prasad was confident that he could help Sebastian.
In 2016, the family made plans to meet the Duke pediatric transplant team. Just days before their departure, Sebastian developed a high fever and a racking cough. His doctors in New York didn’t know what was wrong. Sancho called Dr. Prasad. “He said, ‘Just come on down. Whatever his condition is, we can deal with it better here, and we can take it from there.’”
Duke Cares for Patients and Their Families
“As soon we arrived at Duke, we felt like we were with friends. Dr. Prasad, the team, the nurses were just phenomenal, so caring. We felt truly loved by the whole team,” said Morton. The center strives to make all families feel this way. Dr Prasad explained, “We take care of the patient and the whole family physically, emotionally, in any way they need. That’s one thing that distinguishes us from other centers. We want them to feel supported since they are already dealing with so much worry and anxiety about the transplant.”
"We take care of the patient and the whole family physically, emotionally, in any way they need. That’s one thing that distinguishes us from other centers."

Medical Expertise at Duke
The breadth of Duke’s medical expertise is another factor that distinguishes it from other centers. They have performed thousands of transplants for almost ninety unique diagnoses using bone marrow, umbilical cord blood, or peripheral blood stem cells. Today they “do transplants for diseases that are so rare that many transplant centers haven't even seen them,” said Dr. Prasad. In Sebastian’s case, Dr. Prasad and his team diagnosed and treated Sebastian’s lung problem -- granuloma, a hallmark of severe CDG.
The Transplant Process
When he recovered, the team agreed that Sebastian could undergo the transplant process, which involves chemotherapy to destroy unhealthy cells, the infusion of stem cells, and recovery. Although the side effects from chemotherapy were difficult, recovery was almost as bad. It meant two weeks of waiting to see if the donor cells would engraft or grow new bone marrow cells.
Feeling Like Himself
Thirteen days after the transplant, Sebastian began to feel better. His mom remembers his excitement at celebrating his sister’s birthday in his hospital room. “I just remember being shocked that he was able to have fun and be happy,” she said. “The next day we found out he had engrafted. It was miraculous because it seemed like he was at death's door two days before.”
Today, nine-year-old Sebastian is full of life, and according to Dr. Prasad is “cured of the disease because of the transplant he had at Duke.” Sancho, who has written a book on the entire experience, agreed. “He doesn't take any medications. He doesn't have to have any environmental restrictions. It's like it never happened.”