Natalie Williamson’s hearing loss affected many aspects of her life, leaving her vulnerable and lonely. She couldn’t hear her cell phone ring or her smoke alarm. She rarely left home because conversations with friends and family were too difficult. That all changed after she receive a cochlear implant at Duke Health in 2021. “Unless you’ve lost your hearing and then it’s given back to you, it’s difficult to understand how life-changing it is,” said Williamson, who is 58 and lives in Goldsboro, NC. Today, she’s grateful she can do things she couldn’t do before, like chatting with friends in a restaurant and listening to music. “Having that sense back is priceless.”
The Shock of Sudden Hearing Loss
One Sunday morning in 2005, Natalie Williamson woke up to realize she couldn’t hear out of her left ear. The next day, she was diagnosed with sudden sensorineural hearing loss – a rapid loss of hearing in one ear that can be due to a viral infection of the inner ear.
Over time, Williamson started losing hearing in her right ear, likely due to aging. It wasn’t until her kids moved away from home that Williamson realized how much she relied on them to help her hear. That’s when she began researching cochlear implants.
How Cochlear Implants Restore Hearing
Cochlear implants are surgically implanted devices that transmit sound to the brain using electrical impulses. They create a new way for the brain to hear and translate sound.
“With a cochlear implant, unlike a hearing aid, we’re not relying on existing function,” said Howard Francis, MD, a Duke ear, nose, and throat (ENT) doctor and otologist/neurotologist who specializes in treating complex ear problems. “We bypass the hair cells or sensory receptors, and we place an electrical device next to the auditory nerves that are sitting at the center of the cochlea in the inner ear. When stimulated by electrodes, they deliver coded information to the brain for processing, perception, and understanding.”
Finding the Best ENT for Cochlear Implantation
Williamson wanted a surgeon with top-notch education and expertise. She found it in Dr. Francis, who has more than 20 years of experience with cochlear implantation surgery. After a thorough evaluation by Dr. Francis and Duke audiologist Heather Toth, Williamson underwent the surgery in April 2021.
The Real Work Begins
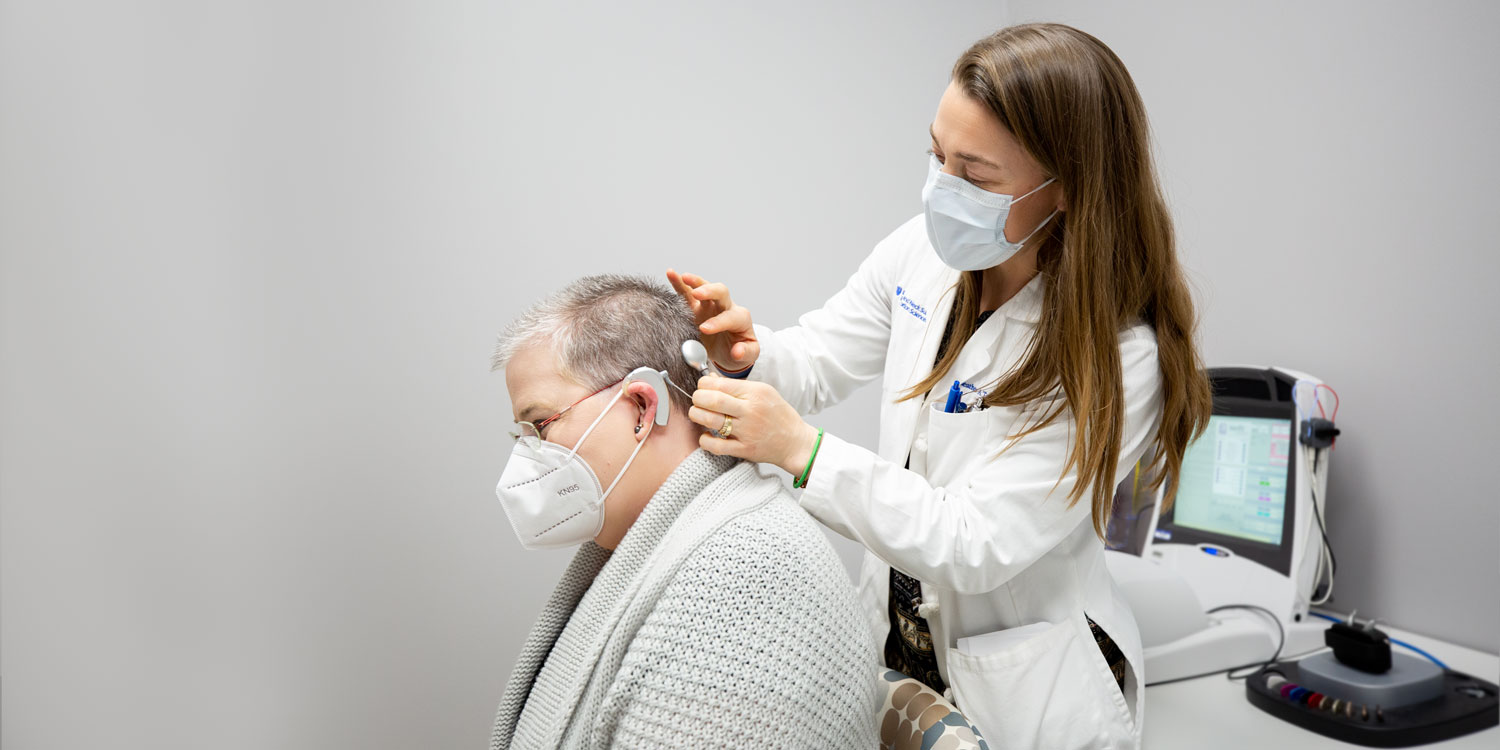
Six weeks later, her incision was fully healed, and Williamson was ready for the device to be turned on or “activated.” One month after activation, Williamson’s hearing had improved to 77%, up from just 3% before her cochlear implant surgery. Toth and Duke speech pathologist Sarah Stidham worked closely with Williamson to fine-tune the implant and help her adjust to it. That process is called aural rehabilitation.
“The hardest part of cochlear implantation is learning how to use it,” Toth said. Two things speed up the process: wearing the device as much as possible and practicing with the device. Because she was so committed to practice, Williamson made quick progress. “Everything they told me to do, I did,” she said. “I followed their instructions, I did all of their exercises, I put my heart and soul into it.”
Duke audiologist Heather Toth adjusts Williamson’s cochlear implant.
The Sound of Gratitude
Today, thanks to the cochlear implant in her left ear and a hearing aid in her right ear, Williamson can locate where a sound is coming from (called sound localization or spatial hearing). This gives her greater awareness of her surroundings. She can also understand speech, even amid background noise. Williamson can barely contain her gratitude. “There were three things I wanted out of this journey,” she said. “To be able to hear my father, to be able to hear my children, and to be able to hear music. I have gotten that and so much more.”
According to Dr. Francis, cochlear implantation can help more people than ever, thanks to recently expanded eligibility criteria that include people with single-sided deafness. “The cochlear implant is one of the most important medical developments to have occurred in the 20th century,” Francis said. “It’s transformative, and Natalie embodies that.”