Fayetteville artist Stephanie Bostock didn’t know how advanced her thyroid cancer was when she was first diagnosed. But she knew she needed to find experienced doctors to treat her.
Perhaps it was her keen artist's eye that led Bostock to notice the lump that had developed in her neck. “I was looking at myself in the mirror,” she said. “Something seemed different.” When her gynecologist noticed it too, he ordered an ultrasound, which indicated the lump was a large nodule on her thyroid gland.
Bostock’s next stop was an ear, nose and throat (ENT) specialist, who ordered a biopsy. He told her not to worry, since most thyroid nodules aren’t cancerous. “He said he’d only seen a handful of cases of cancerous thyroid nodules in his whole career,” Bostock said.
When the biopsy revealed the nodule was thyroid cancer, the ENT wanted to operate immediately. Instead, Bostock recalled thinking, “‘I have to see somebody who knows more about this.’”
The Importance of a Thorough Evaluation
After researching her options, Bostock made an appointment with Sanziana Roman, MD. “The moment I met her, I knew she would help me through this,” Bostock said. “She was very thorough. She was easy to communicate with. She answered all my questions.”
Roman is an endocrine surgeon specializing in thyroid diseases who has treated more than a thousand thyroid cancer patients. “It really is a matter of experience,” Roman said. “Patients can present in different ways with different types of diseases of the thyroid gland. Understanding the biology of each of them is very important in assuring patients get the right care.”
Roman ordered neck mapping, an ultrasound exam of the lymph nodes in Bostock’s neck to determine if—and where—the cancer might have spread. The suspicious lymph nodes were biopsied, too. Results showed the cancer had spread from Bostock’s thyroid into her lymph nodes.
“A thorough evaluation of the extent of the thyroid cancer before surgery is paramount,” said Roman, who added that it’s the most important step in treating thyroid cancer. “Knowing how extensive the cancer is and how much of the thyroid needs to be removed allows patients to get neither too little nor too much surgery,” she said. While this approach is routine at Duke, it’s not the case everywhere. “I see a lot of patients who have had surgeries which are not comprehensive, and then risky repeat surgeries need to be done,” Roman said.
In September 2014, Bostock underwent extensive surgery during which Roman removed her thyroid and more than 50 lymph nodes; 36 of them contained cancer. “She saved my life,” Bostock said of Roman.
Follow-up Treatment Seeks to Foil Cancer’s Return
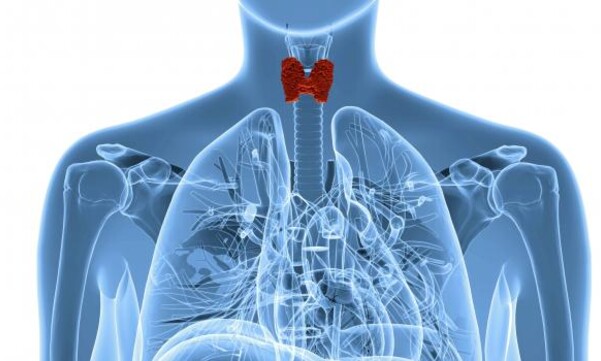
The thyroid gland is located in your throat, near delicate structures that help you eat, talk and breathe. That makes it difficult for surgeons to remove all your thyroid tissue. Thyroid cells left behind could be, or can later become, cancerous. So an additional treatment that involves swallowing a radioactive form of iodine often follows surgery. Ideally, any remaining thyroid cells—the only ones in your body that take up significant amounts of iodine naturally—absorb the radioactive iodine and are destroyed from within.
Because Duke endocrine surgeons and endocrinologists also help develop advances in thyroid cancer treatments, Bostock was able to participate in a clinical trial of a new medication designed to enhance the effects of her iodine treatment. “It was a good opportunity for someone like me, since I’m considered at high risk for reoccurrence,” Bostock said.
Keeping Watch
Bostock has completed treatment and is now in a wait-and-watch mode under the careful management of Duke endocrinologist Jennifer Perkins, MD. Perkins monitors Bostock’s levels of thyroglobulin, a tumor marker produced by thyroid cells. “Even though her tumor markers aren’t at zero, we haven’t seen any new tumor growth on her scans,” said Perkins. “Many patients experience this, but as long as they have close surveillance, they still often have excellent outcomes.”
In the meantime, Bostock is glad to have a team of Duke experts on her side. “There’s not just one person who’s trying to help me with my situation,” she said. “My oncologist talks to my endocrinologist, who talks to my endocrine surgeon. They communicate; they look at my scans together.”
That team approach is by design at Duke Endocrine Neoplasia Center. Said Perkins, “When you have communication between different care providers who have different expertise, you get the benefit of many doctors’ knowledge. Our goal is to offer that in a one-stop shop, where we address all patient concerns with the needed level of expertise in one place, on one day.”
Giving Expression to Cancer’s Impact
Bostock says her experience with thyroid cancer prompted her to devote more time and energy to her lifelong interest in painting.
“Painting allows me to express myself on canvas,” she said. “For me, it’s a meditation and an outlet.” Her passion has turned into a small business, with a website where she sells her works and writes a blog—occasionally about her thyroid cancer experience.