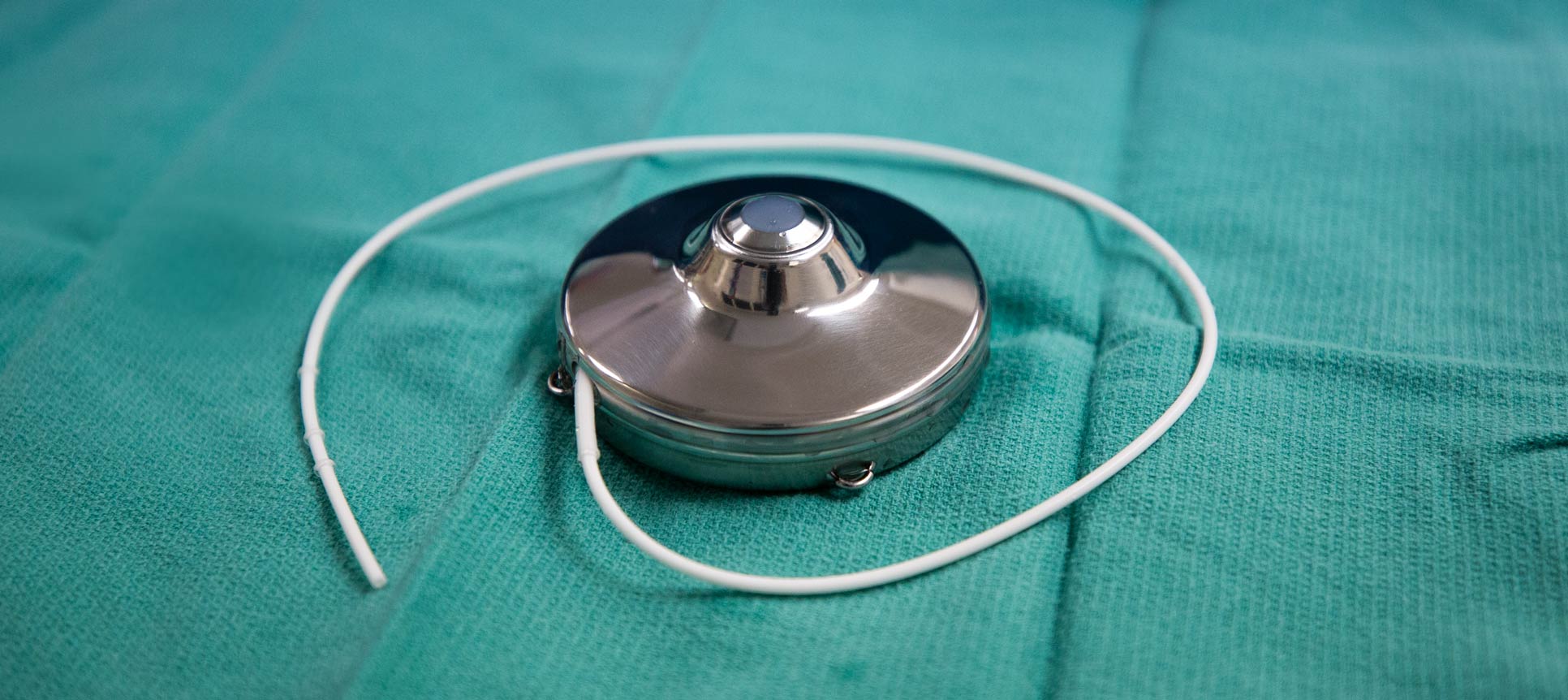
A chemotherapy infusion pump may be a treatment option for people whose metastatic colorectal cancer has spread to the liver, including those who may have been told they are out of options. Duke Health surgical oncologists were the first to implant the hepatic artery infusion (HAI) pump after it received FDA approval. At the time, they were among the few U.S. surgeons with the training and expertise to offer this highly specialized treatment. Now, Duke surgeons are leading the field through an international collaborative and by chairing national clinical trials.
“Most people are looking to live as long as possible with the best quality of life,” said Michael Lidsky, MD, a Duke Health surgical oncologist who performs the procedure. “Hepatic artery infusion may give them that. While the therapy has been around for decades, we are finally running the critical trials to truly determine the impact of HAI in the modern era.”
The Role of Hepatic Arterial Infusion
When colorectal cancer spreads, it frequently results in metastatic tumors in the liver. When possible, the liver tumors are surgically removed, and chemotherapy destroys the remaining cancer cells. Sometimes the tumors can’t be removed because of their location or size, or the available treatments simply can’t slow the disease. At this point, some people are told by their doctors that chemotherapy is their only option. Or worse, that nothing more can be done. However, HAI may be an alternative therapy for some patients.
Hepatic arterial infusion delivers chemotherapy through a pump that’s implanted in the abdominal wall. “We then use a catheter to deliver high doses of chemotherapy through the hepatic artery, which directly feeds metastatic tumors in the liver,” said Peter Allen, MD, a Duke surgical oncologist. Even though the HAI pump delivers chemotherapy directly to the liver at concentrations that are hundreds of times higher than whole-body chemotherapy, it does not increase the side effects beyond those associated with whole-body chemotherapy.
If the liver tumors can be removed -- doctors use the term “resected” -- the pump may be implanted at the time of surgery and used to delay or prevent recurrence of cancer. If the liver tumors cannot be removed, the pump may be inserted to help control the tumor or, even better, shrink its size so it can be surgically removed in the future.
Duke Surgeons’ Expertise with HAI Pumps
Drs. Lidsky and Allen and their Duke colleagues have implanted more than 200 pumps in people with liver metastases from colorectal cancer since they started offering the procedure in conjunction with whole-body chemotherapy in late 2018. In many cases, they use a robotic approach to implant the pump, a technique that was brought to Duke with the help and expertise of surgical oncologist Sabino Zani, MD. The minimally invasive approach, which requires smaller incisions than traditional surgery, allows people to spend less time in the hospital, and recover faster.
Duke Leads the Way in Expansion of HAI
Dr. Lidsky, who leads the Duke HAI Team, also co-leads a consortium of HAI programs around the world. Together, they are advancing the field by providing instruction, mentorship, and support to new centers so they can establish safe, effective, and sustainable programs; analyzing outcomes to learn more about who the best candidates are; and identifying opportunities to make it safer and more effective, and, importantly, executing modern-day multi-center clinical trials.