No one likes to discuss colon health, but it’s serious business. Learning how to take care of your colon can help ensure you and your loved ones lead healthier lives.
Karen L. Sherman, MD, MS, a colorectal surgeon and surgical oncologist with Duke Colon and Rectal Surgery of Raleigh, treats every condition you don’t want to talk about -- from hemorrhoids and fecal incontinence to colon and rectal cancer and diverticulitis. Dr. Sherman offered these colon health tips.
Q. What’s the most important thing to do for colorectal health?
A. The best approach to good colorectal health is to maintain a high-fiber diet and drink plenty of water. Aim for eight glasses of water a day to help prevent constipation. A high-fiber diet will help prevent complications of hemorrhoids, anal tears, and diverticular disease.
Q. Should I get a colonoscopy?
A. Everyone should have a screening colonoscopy starting at age 50 -- or earlier, if you have a family history of colon or rectal cancer. Most health insurances cover it. Colonoscopy allows your doctor to identify and remove benign polyps before they turn into cancer. Waiting until you have symptoms could mean cancer is diagnosed at a later stage. If you develop symptoms such as a change in your bowel movements or rectal bleeding, you should talk with your doctor about a colonoscopy. Catching a cancer early leads to a better prognosis.
Q. Most people know that surgery is used to treat colorectal cancer, but what other conditions do you treat with surgery?
A. Surgery is necessary to treat recurrent or complicated bouts of diverticulitis and inflammatory bowel diseases that don’t respond to other treatment. It is also used to treat benign problems of the anus and rectum when conservative approaches haven’t worked.
Q. Does surgery leave a scar?
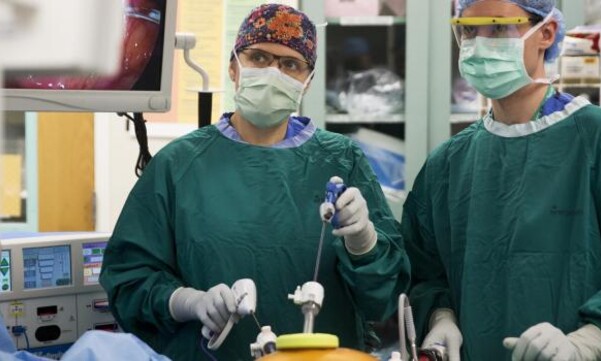
A. We specialize in minimally invasive surgery, including laparoscopic, and single-site surgeries, which leave patients with smaller scars, less pain, and a faster recovery. There is no scar from transanal surgery, since all work is done through the anus.
Q. Why do we get hemorrhoids, and what kinds of problems can they cause?
A. Everyone has hemorrhoids; they’re part of our normal anatomy. It’s just a question of whether they’re bothering you. Hemorrhoids can become aggravated with changes in bowel habits, such as diarrhea and constipation. Over the years, they can pull away from the underlying muscle, descend from the body (prolapse), or bleed. Hemorrhoids can cause pain, itching, bleeding, or prolapse. Pregnancy can also cause hemorrhoids to become problematic because of increased pelvic pressure.
Q. How are hemorrhoids treated when they become aggravated?
A. Initial management includes increasing the amount of fiber and water in your diet. Most of my patients find that’s all they need. I recommend 25 to 30 grams of fiber a day. That’s difficult to achieve through diet alone, so I recommend adding over-the-counter fiber supplements. These come in powders that you can mix with liquid and drink, wafers, or capsules. Look for the active ingredients psyllium husk or methylcellulose. If adding fiber to your diet doesn’t work, there are simple and painless office procedures to treat hemorrhoids. If these fail, surgery may be the next step.